What is LAVAT?
What is LAVAT?
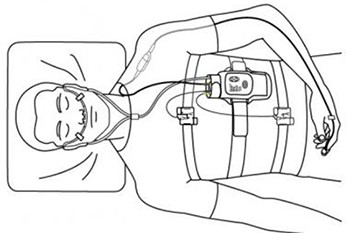
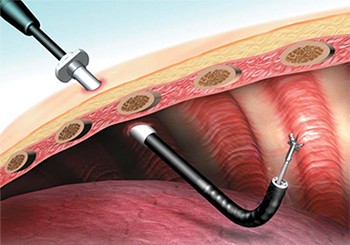
Medical thoracoscopy, or local anaesthetic video assisted thoracoscopy (LAVAT) is a day procedure, performed in the hospital, to allow further assessment of pleural fluid collections and pleural diseases.
Why LAVAT?
- LAVAT has similar indications to Video Assisted Thoracoscopic Surgery (VATS), however, it is less invasive, with fewer incisions and less requirement for anaesthetic.
- It allows : visualisation of the pleural lining, safe drainage of large volumes of pleural fluid (with a lesser risk of re-expansion pulmonary oedema), lysis of simple adhesions, and performance of guided pleural tissue biopsies the insertion of intra-pleural talc, to enable pleurodesis, with the intent of preventing further re-accumulations of pleural fluid.
Who is right for LAVAT?
It is often considered in patients for whom ultrasound guided fluid aspirations have failed to reveal a likely diagnosis. It is not appropriate for patients in whom more invasive surgery is required.
What is Involved?
- LAVAT is often performed under conscious sedation.
- Admission to hospital may be required depending upon whether a pleurodesis is performed, or complications (which are rare) occur.
Medical thoracoscopy was initially performed in 1910 by an internist from Sweden, Hans-Christian Jacobaeus. Jacobaeus was the first to use the term thoracoscopy, which he described as “replacing fluid with air” in order to examine the pleural surfaces of two patients with tuberculous pleurisy. Jacobaeus later developed a therapeutic application for thoracoscopy by using thermocautery to lyse adhesions and create a pneumothorax to treat tuberculosis.
During the 1950s and 1960s, thoracoscopy gained popularity with pulmonologists because of the tuberculosis endemic in the United States. The major indications were for pleural and pulmonary biopsies for diffuse lung disease. However, with the advent of effective chemotherapy for tuberculosis, the need for thoracoscopy decreased. The procedure was later adopted by surgeons after advances in optics, laparoscopic techniques, and video technology. Thoracoscopy grew into the video-assisted thoracoscopic surgery that is currently performed by thoracic surgeons.
The term thoracoscopy is confusing because it refers to both the medical and surgical procedures. To avoid confusion, some authors suggest that medical thoracoscopy should be referred to aspleuroscopy. The term thoracoscopy may be used exclusively for the surgical thoracoscopic procedure.
Indications
The accepted indications for medical thoracoscopy include the following
- Workup and diagnosis of idiopathic pleural effusions.
- Staging of lung cancer.
- Pleurodesis.
- Site-directed biopsy of parietal pleura.
- Staging for mesothelioma.
Idiopathic pleural effusions that have been sampled by thoracentesis are ideal for medical thoracoscopy. The direct visualization of the pleura allows for site-directed biopsy of abnormal parietal pleura. Additionally, it allows for examination of the visceral pleura and any clues that may provide towards the diagnosis of the pleural effusion. Currently, most interventional pulmonologists limit biopsy to the parietal pleura due to the risk of injury to the lung when sampling the visceral pleura.
Pleural Effusion of Unknown Origin
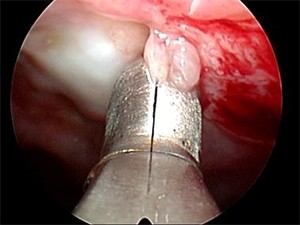 Cytologic examination of pleural fluid is only diagnostic in 60-80% of patients with metastatic pleural involvement and in less than 20% in patients with mesothelioma.[2] In cases for which the initial evaluation of a pleural effusion is nondiagnostic and malignancy is suspected, medical thoracoscopy and parietal pleural biopsy should be considered. Medical thoracoscopy with pleural biopsy, as shown in the image below, establishes a diagnosis in more than 90% of the cases.
Cytologic examination of pleural fluid is only diagnostic in 60-80% of patients with metastatic pleural involvement and in less than 20% in patients with mesothelioma.[2] In cases for which the initial evaluation of a pleural effusion is nondiagnostic and malignancy is suspected, medical thoracoscopy and parietal pleural biopsy should be considered. Medical thoracoscopy with pleural biopsy, as shown in the image below, establishes a diagnosis in more than 90% of the cases.
Malignant Pleural Effusion/Pleurodesis
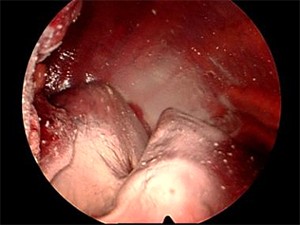
In cases with an established malignant diagnosis, medical thoracoscopy also has a therapeutic role in the form of pleurodesis. Complete evacuation of pleural fluid, with maximization of lung expandability by removing adhesions and pleurodesis by talc insufflations (see the image below), has short- and long-term success rates greater than 90%.
 The benefit of the pleurodesis is twofold. First, it improves the patient’s functional status and quality of life. In the setting of advanced malignant disease, this is the central goal of any physician. In patients who are undergoing further treatment for malignancy, there is an added benefit of increasing treatment options by improving the patient’s functional status.
The benefit of the pleurodesis is twofold. First, it improves the patient’s functional status and quality of life. In the setting of advanced malignant disease, this is the central goal of any physician. In patients who are undergoing further treatment for malignancy, there is an added benefit of increasing treatment options by improving the patient’s functional status.
In addition, patients who do require further treatment can be excluded from certain chemotherapeutics because of the chemotherapy’s tendency to distribute into the pleural effusion and affect serum levels. The classic examples of this are methotrexate, fludarabine, and possibly pemetrexed.
Survival of patients with advanced pleural disease is often discussed in weeks to months. The benefits of medical thoracoscopy against repeated thoracentesis should be carefully considered for the individual patient.
Lung Cancer
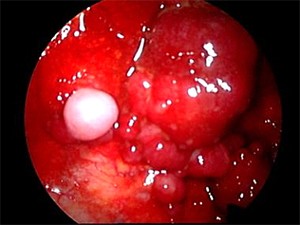 In the patient with known lung cancer and an effusion with a negative cytology, medical thoracoscopy is an excellent tool. It allows for direct visualization of the pleura and a thorough examination for evidence of metastasis (see the images below).
In the patient with known lung cancer and an effusion with a negative cytology, medical thoracoscopy is an excellent tool. It allows for direct visualization of the pleura and a thorough examination for evidence of metastasis (see the images below).
The sensitivity of pleuroscopy-guided biopsy in malignant pleural effusions is 95%, compared to 62% for cytology from thoracentesis and 44% for closed pleural biopsy.[7] By allowing for more accurate diagnosis and staging, this may help prevent unnecessary procedures on a patient who is inappropriately categorized into a lower stage.
Malignant Mesothelioma
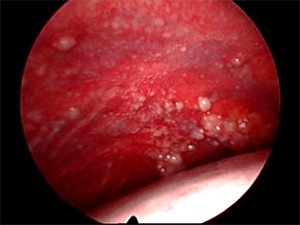 The yield of cytology for malignant mesothelioma is even lower than most malignant effusions, as low as 41% in one study.[8] It can be difficult to reach a definitive diagnosis without complete visualization of the pleural space. Medical thoracoscopy is favored over thoracotomy for two reasons. First, the pleural specimen obtained with the minimally invasive 5-mm forceps is comparable to the specimen achieved with open biopsies. Second, the site-directed nature of pleural biopsies through the semirigid pleuroscope allows a minimally invasive approach.
The yield of cytology for malignant mesothelioma is even lower than most malignant effusions, as low as 41% in one study.[8] It can be difficult to reach a definitive diagnosis without complete visualization of the pleural space. Medical thoracoscopy is favored over thoracotomy for two reasons. First, the pleural specimen obtained with the minimally invasive 5-mm forceps is comparable to the specimen achieved with open biopsies. Second, the site-directed nature of pleural biopsies through the semirigid pleuroscope allows a minimally invasive approach.
Tuberculous Pleural Effusion
There is controversy whether medical thoracoscopy is warranted when the suspicion for tuberculosis is high. In these cases, the diagnostic yield from closed-needle pleural biopsy is approximately 69%, with some studies reporting rates as high as 88%.[3] The current consensus is that medical thoracoscopy should be reserved for special circumstances, such as lysis of adhesions or more effective drainage of loculated effusions, as well as when larger quantities of tissue are needed for sensitivities.
Recurrent Pleural Effusions of Benign Origin
Recurrent pleural effusions are often caused by heart failure, cardiac surgery, nephritic syndrome, connective tissue diseases, and other inflammatory disorders. When these effusions are not controlled by repeat large-volume thoracentesis, pleural biopsies can be obtained through medical thoracoscopy and pleurodesis can be performed if necessary.
Empyema and Complicated Parapneumonic Effusions
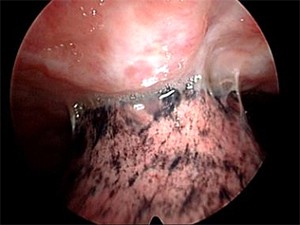 Some interventional pulmonologists have used medical thoracoscopy for drainage of uncomplicated empyema and chest tube placement. Additionally, it can be used carefully for lysis of thin fibrous adhesions (see the image below).
Some interventional pulmonologists have used medical thoracoscopy for drainage of uncomplicated empyema and chest tube placement. Additionally, it can be used carefully for lysis of thin fibrous adhesions (see the image below).
Currently, this is not routinely performed or the standard of care, mainly because timing is key in these procedures and they should be considered early if chest tube drainage is inadequate. In later phases of the empyema, there may be thick fibrous adhesions, pleural peel, or trapped lung. In these cases, early video-assisted thoracoscopic decortication is required.
Pneumothorax
Medical thoracoscopy can offer definitive treatment or diagnostic inspection of a patient with a recurrent pneumothorax. In patients who are not candidates for video-assisted thoracoscopic surgery, pleural abrasion or talc pleurodesis can be performed. For patients suitable for video-assisted thoracoscopic surgery, bullectomy, pleural abrasion, and pleurectomy in the operating room are superior and preferred.
Contraindications
The major contraindications are related to the ability to perform the procedure. As long as no contraindication exists for the ability to insert instruments into the pleural space, it can be performed safely. Even when the lung is adherent to the chest wall, the use of transthoracic ultrasound by interventional pulmonologists can allow identification of safe areas to insert the trocar and pleuroscope.
A pleural separation of at least 10 mm is recommended to minimize injury to the lung. In patients with small effusions, a pneumothorax may need to be induced by cannulating the pleural space and asking the patient to inspire deeply while the catheter is open to the atmosphere. The presence of a pneumothorax can then be confirmed with either chest radiograph or thoracic ultrasound at the bedside. This procedure is limited by the ability of the patient to tolerate a pneumothorax. In patients who already have an effusion, the concern regarding tolerance of a pneumothorax is not as worrisome because an equal volume of fluid would be replaced by air.
The following relative contraindications may be corrected and accounted for:
- Refractory cough
- Hypoxia
- Coagulopathy
- Thrombocytopenia